In a managed-care plans setting (PPO, DMO), the patient is usually asked to choose his/her dental care provider from a list of the plan’s preferred providers. This is a term used to describe dentists who contract with the dental benefit plan. Choosing your dentist from this group may or may not affect your levels of reimbursement. Most people don’t understand the reimbursement level on their dental bill. Here are some features that are commonly misunderstood:
Yearly Maximum
The entity who purchased your dental benefits plan (usually, your employer’s HR) makes the final decision on “maximum levels” of reimbursement through the contract with the insurance company; it is often based on the amount the employer wishes to pay for the dental benefit. Even though the cost of dental care has increased significantly over the years, the maximum levels of insurance reimbursements have remained the same since the early 1970s. Only a few plans offer higher maximums that are keeping up with rising dental care costs.
Deductible
Most people with dental insurance are unaware that they may have to pay a deductible. A deductible on a dental policy is the fee you agree to pay in the event you get dental work, and they are usually due annually. It usually is between $50 and $250, and it works this way, after you pay up to the value of your deductible, the dental insurance starts paying your benefits. For example, if you have a $50 deductible and your first dental visit for the year costs $150, you will owe $50 of the bill; your insurance company will owe the remaining $100. Then, the next bills will be covered base of your coverage dental benefits percentage. It is good to always be aware of what deductible is being offered on a dental insurance policy before you buy it. Then, make sure you are willing to pay that amount.
Customary and Reasonable
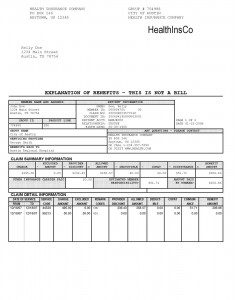
UCR (Usual, Customary and Reasonable) is one of the most misunderstood terms used to describe dental benefit plans. This is a term made up by the insurance company; UCR plans pay an agreed upon percentage of the dentist’s fee, or pay what the insurance company deems a “customary” or “reasonable” fee limit, whichever is less. Although these limits are called “customary,” they generally do not reflect the actual set fees of the dentists in your area. In your explanation of benefits (EOB), you may note that your dentist fees are higher than the UCR reimbursement levels that your plan offers. This does not mean that you have been overcharged. There is currently no available regulation as to how insurance companies determine reimbursement levels and they are not required to disclose how they determine these levels. This usually results in wide fluctuations.
Frequency and Age Limits
This is a common cause of problems with patients and insurance coverage. Most dental insurance policies will often have the following frequency limit wording:
- a. One time in six months, i.e. the service is paid once every 6 months, but not one day sooner
- b. Two times per calendar year, i.e. the service is paid for any date of service up to twice in a calendar year
- c. Two times in a twelve month period, i.e. the service is paid twice in a twelve month period, which may include looking back into the prior insurance year
Policies also have different frequencies for specific service types. A common example is fluoride for children. Some policy allow two cleanings in a calendar year, however only one fluoride treatment per year. For better caries prevention, our protocol is to apply fluoride twice per year. In addition, policies who allow fluoride treatments usually have age limits (when the insurance company stop paying for fluoride treatment), which can differ from one policy to another.
Other services may also have time limitations. Some limitations often seen:
- Full series x-rays/panoramic x-rays are often limited to once per 3 or 5 years.
- Fillings are usually limited to once per every two years on the same tooth.
- Crowns and bridges are usually limited to one time per tooth every 5, 7 or 10 years. Even if a crown or bridge breaks.
- Scalings (treatment for periodontal disease) are usually limited to 1 per quadrant per every 2 years on the same quadrant.
Pre-existing Conditions
Just like medical insurance, your dental plan may not cover conditions that existed before you enrolled in the plan. In addition, your plan may not cover certain conditions for which you may need treatment. Your dental plan may, also, not cover certain procedures; this does not mean these treatments are unnecessary. Sealants, for example, protect your teeth from caries and save you money in the future.
Missing tooth clause
If you are missing a tooth and are looking to get a bridge or an implant to replace the missing tooth, your policy may have a ‘missing tooth clause’. This means if you had the tooth extracted prior to enrolling with your current policy, they will not pay any benefits towards restoring that tooth.
Alternate Benefits Provisions
At time, your dental insurance plan may not allow benefits for some treatment options, and suggest another treatment. For example, your dentist may recommend a crown or onlay, but your insurance may offer reimbursement only for a large filling, which can ultimately break or break the tooth. As with other choices in life, the least expensive alternative is not always the best option.
Conclusion
As a courtesy to our patient, our staff will try to assist you as much as possible with your dental insurance, however they may not always be able answer specific questions about your benefits or predict the amount of your coverage for a specific procedure, because plans from the same issuer (Aetna, Cigna, Delta, etc) offered by the same employer may vary greatly according to the contracts involved. Deductible and co-pays for service rendered are always due at the time of service.
Your employer HR usually is in the best position to explain the individual design features of your plan and answer specific questions about your coverage. Also, you can call the customer service department of your dental benefits plan issuer for additional information.






